Burlington, Ontario Guide
Burlington, Ontario Guide(Burlington, Ontario Guide)
If you live in Burlington, Ontario (or nearby; Oakville, Hamilton, Milton, Mississauga, Waterdown, or the Halton Region) and you’ve noticed your posture “doesn’t look like it used to,” you’re not alone. Many people first suspect scoliosis because of subtle body changes—often before pain becomes persistent.
Scoliosis is not just a “teen issue.” It can show up in adolescence during growth spurts, and it can also become more noticeable in adults due to age-related spinal changes. The good news is that early action is where long-term outcomes are built—and a chiropractic-led plan that includes non-surgical spinal decompression can be a powerful way to address the underlying mechanical drivers of scoliosis-related discomfort and mobility limits.
This Burlington-focused article covers:
- What scoliosis is (in plain language)
- The top 5 early signs you shouldn’t ignore
- Why objective imaging matters (not guesswork)
- Why spinal decompression is a cornerstone of long-term, non-surgical care for many scoliosis patients—especially when the curve is linked to uneven disc pressure and nerve irritation

Quick refresher: what “scoliosis” actually means
Scoliosis is a sideways curvature of the spine that’s typically measured on an X-ray using the Cobb angle, however the cobb method of analysis is an old out-dated model of assessment.
A curve greater than 10 degrees is considered scoliosis, and treatment decisions usually depend on the curve magnitude, symptoms, age, and whether the curve is progressing. However it is more complex than it seems.
It’s also important to know scoliosis is often described as a three-dimensional deformity (not just a “C-shape” on a flat image). That 3D element helps explain why posture changes can show up in shoulders, ribs, hips, and balance.
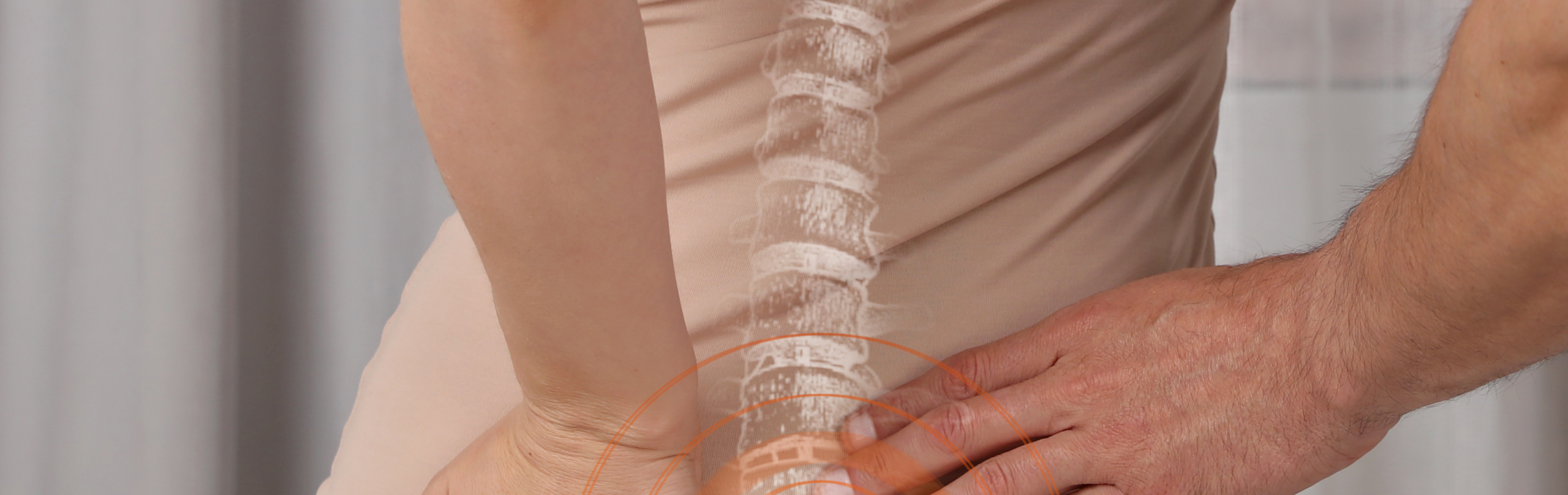
Why early signs matter for long-term results
When scoliosis is noticed early, you have more time to:
- Measure it properly (rather than guessing)
- Identify whether symptoms are coming from the curve itself, uneven disc loading, or nerve irritation
- Build a plan aimed at lasting function (posture, mobility, spinal stability) instead of chasing symptoms
In adults, scoliosis is frequently associated with back pain patterns that can be asymmetric and sometimes radiate into the leg depending on spinal mechanics.
The Top 5 Early Signs You May Need Scoliosis Treatment
1) Uneven shoulders or a “prominent” shoulder blade
One of the earliest signs people notice—often in a mirror, in photos, or when clothing sits oddly—is that one shoulder appears higher than the other, or one shoulder blade looks more pronounced.
What it can mean:
A spinal curve and rotation can shift the ribcage and shoulder girdle, changing how the shoulders sit—even if you feel “fine” otherwise.
Burlington next step (long-term focused):
This is exactly the kind of sign that benefits from a structured assessment rather than guesswork. At Burlington Spinal Decompression, Dr. Brad Deakin starts with a chiropractic-led evaluation and can use on-site digital X-rays to measure structural alignment and plan care precisely.
2) Uneven hips, uneven waistline, or clothes that “hang wrong”
Scoliosis doesn’t just affect the upper body. A very common early clue is:
- One hip appears higher
- The waistline looks uneven
- Pants hems or shirts don’t hang evenly
- You feel like you “stand into” one side
These signs are widely recognized in clinical overviews of scoliosis symptoms.
Why this matters for treatment:
Hips and waist asymmetry often reflects how the curve influences pelvic position, which can create uneven disc pressure and compensations over time—especially in adults who sit long hours or do repetitive work.
3) Rib “hump” or one side of the rib cage sits higher when bending forward
A classic early sign of scoliosis is that when you bend forward, one side of the rib cage appears higher than the other. This is related to the rotational component of scoliosis.
What you might notice in real life:
- Sports bras or shirts twist slightly
- Your back looks uneven in change-room mirrors
- A friend/family member points out asymmetry during a stretch
Why Burlington imaging matters here:
Because scoliosis is measured in degrees, long-term planning starts with objective measurements—not “it looks a bit off.” The Scoliosis Research Society describes X-rays and Cobb angle measurement as standard for evaluating scoliosis. However, this is the old method of analysis, as it is deemed to be inherently flamed.
At Burlington Spinal Decompression, the clinic notes it provides on-site digital X-rays, which helps reduce delays and supports accurate care planning.
4) Persistent back stiffness, fatigue, or asymmetrical “one-sided” pain
Scoliosis isn’t always painful early—especially in kids—but pain and fatigue are common reasons adults finally seek care. Health authorities and clinical resources note that as scoliosis progresses or becomes more severe, it can contribute to back pain.
Research in adults also suggests scoliosis-related pain often presents with asymmetric localization, frequently near the curve’s apex, and can have distinct patterns compared with nonscoliosis back pain.
What “early” can look like in adults:
- You’re “fine” in the morning, but stiffness builds throughout the day
- Standing or walking long periods (work, shopping, events downtown) feels harder than it should
- You constantly shift position to find relief
- Pain is more on one side than the other
Long-term mindset shift:
This is where people often get stuck chasing quick fixes. A better path is a plan aimed at lasting spinal mechanics—reducing uneven compression, restoring movement, and building stability.
5) Leg symptoms (numbness/tingling) or reduced breathing endurance in more advanced cases
While scoliosis can be subtle, it can also influence the spine in ways that irritate nerves—especially in adults where disc and joint changes may accompany the curve. Adults with scoliosis can experience pain that eventually radiates into the leg, and leg symptoms may relate to the structural mechanics present in scoliosis.
In more severe cases, scoliosis can also affect breathing mechanics; reputable clinical sources note breathing difficulty can occur rarely in severe scoliosis.
This sign matters because it often indicates more than “posture.”
When nerve-related symptoms show up, it’s time for a proper assessment and measurement so care decisions are based on facts.
Why chiropractic-led spinal decompression is a long-term answer for many scoliosis patients
Let’s be direct: scoliosis is structural, and there isn’t a single “one-size” solution for every curve. But for a large number of people—especially adults—what drives day-to-day suffering is often the mechanical stress around the curve: uneven disc pressure, joint restriction, muscle imbalance, and sometimes nerve irritation.
That’s where 4- Dimensional non-surgical spinal decompression fits—particularly when delivered as part of a chiropractic-led, structured plan (not as a random standalone session). It can help unwind a scoliosis in 4-Dimentions.
What spinal decompression is (in plain language)
Spinal decompression uses a specialized table to apply controlled, gradual traction forces designed to reduce pressure on discs and nerves. Burlington Spinal Decompression describes its approach as technology-supported, personalized, and integrated with rehabilitation to support spinal alignment and movement patterns over time.
What the evidence says (and how we apply it responsibly)
High-quality research on traction/decompression is mixed depending on the condition being treated. Broad reviews of traction for general low back pain show limited overall impact when traction is used across wide patient groups.
At the same time, other peer-reviewed evidence shows that when decompression/traction is used in more specific clinical presentations, and combined with a structured plan, measurable improvements can be seen:
- A randomized controlled trial found that adding non-surgical spinal decompression to a routine care program improved pain, function, range of motion, and endurance over a 4-week care block (12 sessions) in people with lumbar radiculopathy.
- A systematic review and meta-analysis in Physical Therapy evaluated traction for lumbar radiculopathy and reported benefits in pain/disability outcomes when specific forms of traction were added to care.
How that relates to scoliosis (important and honest):
Not every scoliosis case equals radiculopathy. But many adults with scoliosis also experience disc and nerve-loading patterns that resemble those studied in decompression research. That’s why a measured, imaging-informed plan matters—so decompression targets the right region and the rehab stabilizes the change for long-term function.
Why Burlington Spinal Decompression (and Dr. Brad Deakin) is the Burlington choice for advanced decompression care
If you’re searching phrases like “scoliosis treatment Burlington Ontario”, “spinal decompression Burlington ON”, or “scoliosis chiropractor Burlington”, the differentiator isn’t hype—it’s precision + planning.
Here’s what Burlington Spinal Decompression highlights about how care is delivered locally in Burlington:
- Chiropractic-led care under Dr. Brad Deakin (Clinic Director / Owner) with 20+ years of clinical experience.
- A focus on 4-Dimensional non-surgical spinal decompression and protocols aimed at long-term spinal health.
- On-site digital X-rays, described by the clinic as allowing measurements down to 1/10th of a millimetre, helping avoid off-site delays and supporting accurate planning.
- Additional scans (the clinic notes tools such as EMG and infrared thermography) to help build and monitor care plans.
- Technology that the clinic states can include lateral flexion and axial rotation during decompression, intended to better address spinal curvatures (including scoliosis-related patterns).
“How fast will I notice change?” The 2–4 week milestone (and the long-term plan)
When people are motivated to finally address scoliosis-related discomfort, they usually want two things:
- Proof that the plan is working
- A strategy that holds up for the long run (not a temporary bump)
A realistic, evidence-aligned expectation is that many patients notice meaningful changes within the first 2–4 weeks when care is consistent—especially when disc/nerve pressure is a major driver. In research on non-surgical decompression for lumbar radiculopathy, measurable improvements were observed at the 4-week mark after 12 sessions.
From there, long-term outcomes depend on what happens next: progressing the plan, stabilizing improvements with rehabilitation, and using objective reassessments to ensure you’re building lasting spinal function. Burlington Spinal Decompression describes structured plans commonly spanning multiple weeks (often 8–20 weeks) with progress-based tapering.
What to do next in Burlington if you recognized one (or more) signs
If you saw yourself (or your child) in the signs above, here’s the most productive move:
Book a scoliosis-focused spine assessment that includes measurement
A scoliosis plan should start with:
- A clear history + functional exam
- Imaging when appropriate to measure and track structural findings (Cobb angle is a standard measurement approach)
- A plan that targets the mechanics behind symptoms, not just symptom-chasing
At Burlington Spinal Decompression, the clinic describes a process that includes on-site imaging and individualized care plans guided by clinical findings.
References (APA 7)
Amjad, F., et al. (2022). Effects of non-surgical decompression therapy in addition to routine physical therapy on pain, range of motion, endurance, functional disability and quality of life versus routine physical therapy alone in patients with lumbar radiculopathy; a randomized controlled trial. BMC Musculoskeletal Disorders, 23(1), 255. doi:10.1186/s12891-022-05196-x.
HealthLinkBC. (n.d.). Scoliosis in children and teens.
Mayo Clinic Staff. (2025, April 25). Scoliosis: Symptoms and causes. Mayo Clinic.
McAviney, J., Roberts, C., Sullivan, B., Alevras, A. J., Graham, P. L., & Brown, B. T. (2020). The prevalence of adult de novo scoliosis: A systematic review and meta-analysis. European Spine Journal, 29(12), 2960–2969. doi:10.1007/s00586-020-06453-0.
National Institute of Arthritis and Musculoskeletal and Skin Diseases. (2023, July 1). Scoliosis.
Negrini, S., Donzelli, S., Aulisa, A. G., Czaprowski, D., Schreiber, S., de Mauroy, J. C., et al. (2018). 2016 SOSORT guidelines: Orthopaedic and rehabilitation treatment of idiopathic scoliosis during growth. Scoliosis and Spinal Disorders, 13, 3. doi:10.1186/s13013-017-0145-8.
Scoliosis Research Society. (n.d.). Diagnosing scoliosis.
Vanti, C., et al. (2021). Effectiveness of mechanical traction for lumbar radiculopathy: A systematic review and meta-analysis. Physical Therapy, 101(3), pzaa231. doi:10.1093/ptj/pzaa231.
Wegner, I., Widyahening, I. S., van Tulder, M. W., Blomberg, S. E. I., de Vet, H. C. W., Brønfort, G., Bouter, L. M., & van der Heijden, G. J. M. G. (2013). Traction for low-back pain with or without sciatica. Cochrane Database of Systematic Reviews, (8), CD003010. doi:10.1002/14651858.CD003010.pub5.
World Health Organization. (2023). WHO guideline for non-surgical management of chronic primary low back pain in adults in primary and community care settings. Geneva: WHO.
Zaina, F., Marchese, R., Donzelli, S., Cordani, C., Pulici, C., McAviney, J., & Negrini, S. (2023). Current knowledge on the different characteristics of back pain in adults with and without scoliosis: A systematic review. Journal of Clinical Medicine, 12(16), 5182. doi:10.3390/jcm12165182.
Burlington Spinal Decompression. (n.d.). Clinic pages and educational resources (services, technology, conditions treated, and care process).

Burlington Spinal Decompression: Where to find us & how to start
Burlington Spinal Decompression (Dr. Brad Deakin)
Address: 1‑3350 Fairview St, Burlington, ON L7N 3L5
Phone: (289) 337‑9969
We provide on‑site digital X‑rays, advanced nerve scans, and 4‑Dimensional decompression with individualized chiropractic‑led care plans to resolve the underlying issue—so you can get back to what you love. burlingtonspinaldecompression.ca+1
Ready to get started? Book your initial exam today—our team will review your imaging and map a plan to herniated disc relief that fits your schedule and goals. burlingtonspinaldecompression.ca
